If you struggle with lower-face breakouts, your biggest frustration is likely the relentless timeline. You follow your evening double-cleansing routine perfectly, apply your spot treatments, and finally watch a painful lump on your chin begin to shrink. But just as the swelling flattens, a deep, familiar ache begins throbbing millimeters away. Every three to four days, a fresh blemish emerges in the exact same localized zone.
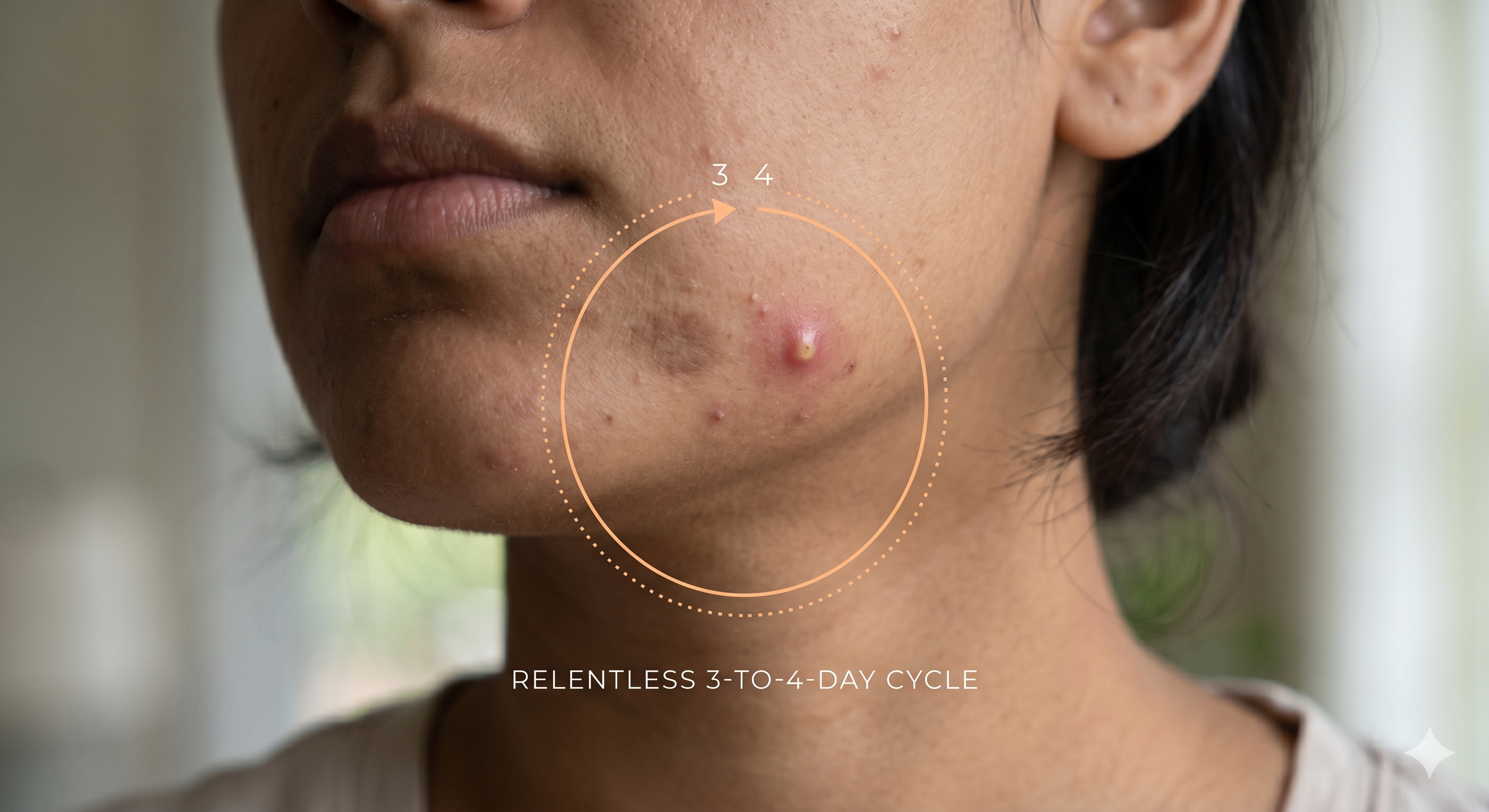
Many people assume their skin is simply purging, or that their active serums have stopped working. However, when breakouts cycle every few days along the chin and jawline, it points to a specific chain reaction happening beneath the surface:
- Subclinical Clustering: Pores in the highly active lower face rarely clog individually. Instead, excess oil and microscopic dead skin cells create a field of invisible, clogged pores (microcomedones) clustered closely together.
- The Inflammatory Domino Effect: When one deep blemish flares up, the localized swelling and immune response place immense physical pressure on the weakened pore linings right next door.
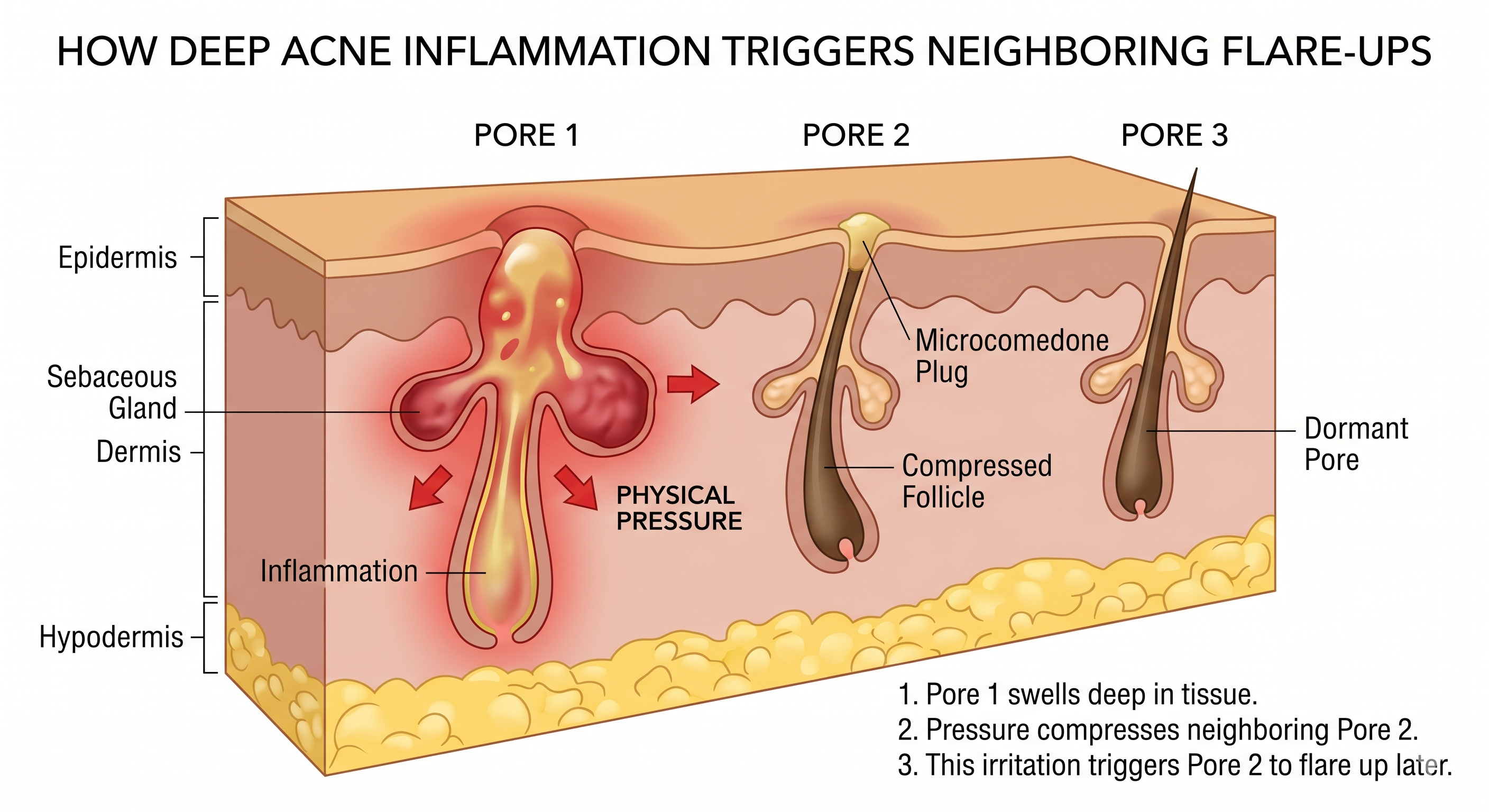
- Staggered Surfacing: Because these trapped pockets sit at varying depths within the skin tissue, they do not mature all at once. As one clears, the internal pressure pushes the neighboring microcomedone over the edge, creating a continuous, staggered loop of visible flare-ups.
To break this cycle, you must stop treating individual spots reactively and audit the internal and external triggers feeding the entire zone.
Before applying active ingredients, perform a structured evaluation of your breakouts using these four diagnostic pillars. Gently washing your hands and evaluating the physical feel of the blemish reveals its depth and structural stage:
Firm, Deep Knots (No Surface Cap)
If the blemish feels like a hard underground pebble that aches even when your face is resting, you are dealing with a deep inflammatory blemish. The pore wall has ruptured deep inside the tissue, and your body has built a thick cellular wall around it.
Diagnostic Action: Squeezing is strictly off-limits; surface physical extractions cannot reach the core.
Soft, Yielding Swelling
Indicates an internal fluid sac tracking deeper in the skin.
Diagnostic Action: Requires gentle soothing to allow the trapped fluids to process naturally.
Superficial Raised Domes
Tiny, clustered surface bumps that feel rough but lack deep throbbing pain point toward superficial pore blockages or localized skin barrier irritation.
Where the blemishes concentrate along the lower face provides crucial clues to their origin:
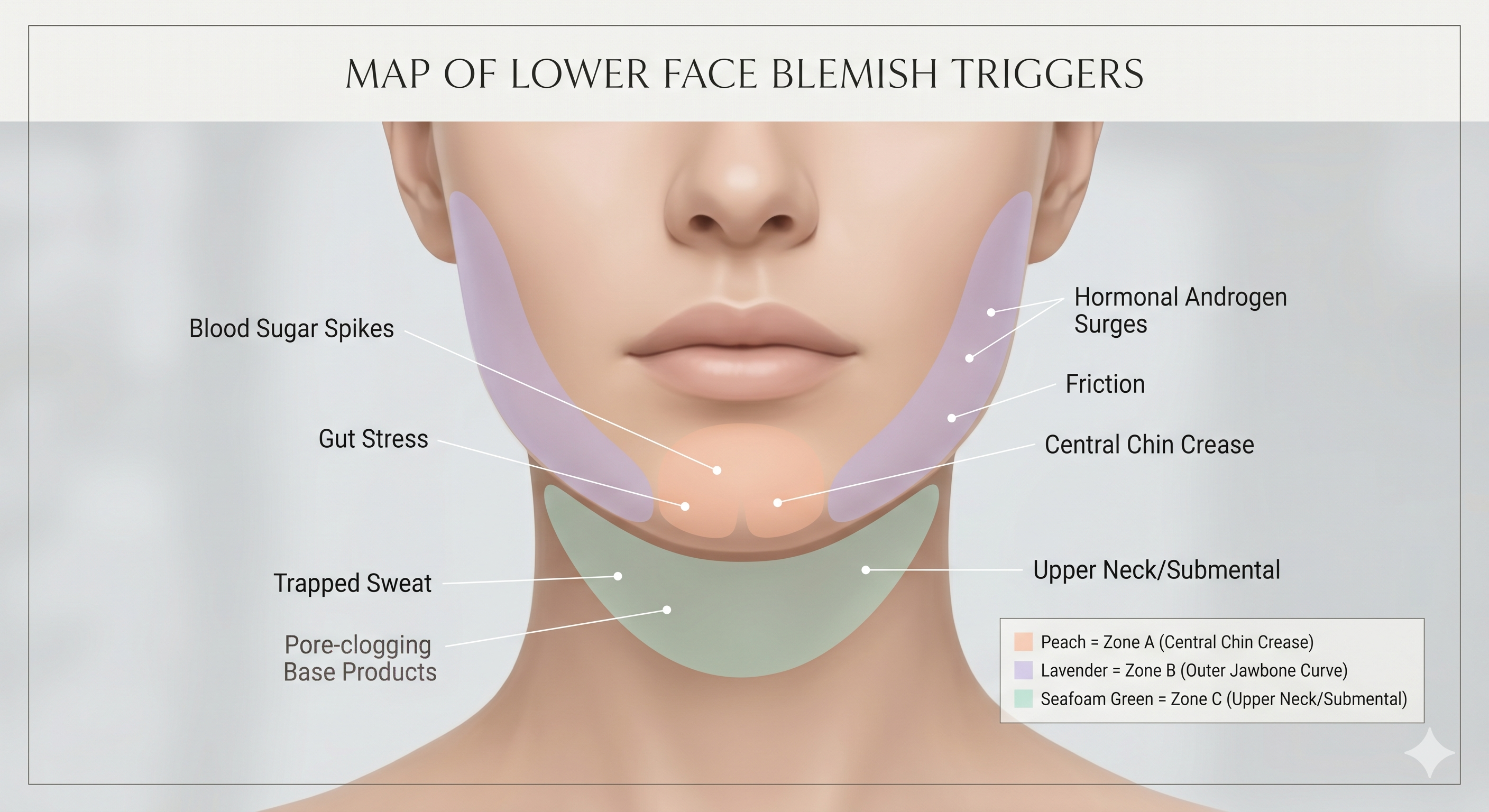
- The Central Chin Crease: Highly dense in sebaceous glands. Constant flare-ups here frequently align with rapid blood sugar fluctuations, digestive stress, or localized sweat pooling.
- The Outer Jawbone Curve: Breakouts tracing the hard line of the jawbone are heavily associated with deep internal androgen surges, as well as repetitive friction from resting the face in unwashed hands.
- The Upper Neck & Submental Area: Blemishes tucked directly beneath the chin line often indicate comedogenic base products, heavy sunscreens that have trapped sweat during peak daily heat, or incomplete evening makeup removal.
Tracking exactly when flare-ups trigger allows you to isolate systemic patterns:
- The Cortisol Connection: High daily stress triggers sustained spikes in cortisol. This hormone directly binds to receptors in your sebaceous glands, commanding them to pump out heavy, thick sebum that easily solidifies inside the lower-face pores.
- Climate Humidity & Trapped Heat: Warm, highly humid environments naturally accelerate baseline oil production. Layering thick, occlusive traditional creams or heavy long-wear foundations over active lower-face zones prevents natural sweat evaporation, leading to rapid bacterial overgrowth.
Diagnostic auditing must evaluate everyday nutrition, as gastrointestinal inflammation frequently mirrors directly onto the lower third of the face.
- Blood Sugar & Insulin Spikes: Regularly consuming highly processed foods, refined flours, and concentrated sweets causes rapid spikes in blood glucose. To process this, the body releases high levels of insulin and insulin-like growth factor 1 (IGF-1), both of which trigger an immediate surge in skin oil production and cellular shedding.
- Dairy Sensitivity: For many individuals, proteins and natural hormones present in heavy dairy products stimulate localized inflammatory pathways, frequently showing up as stubborn, deep swellings along the chin crease.
It is vital to determine whether your lower face is experiencing true internal breakouts or external contact irritation (acne mechanica).
| Diagnostic Clue | Internal / Hormonal Breakout | Mechanical Friction / Irritation |
|---|---|---|
| Primary Appearance | Single or staggered deep, aching lumps. | Dense clusters of uniform, tiny surface bumps. |
| Pain Profile | Deep, lingering ache or sharp throbbing. | Surface itchiness, stinging, or raw sensitivity. |
| Common Triggers | Stress spikes, cycle timing, high-sugar diets. | Chin-resting habits, tight mask straps, unwashed makeup tools. |
| Behavior | Stubbornly lingers for weeks per blemish. | Flairs up rapidly after contact; responds quickly to soothing barrier care. |
Searchers frequently ask if topicals alone can clear persistent chin and jawline concerns. Use this matrix to determine your next steps safely:
When to Optimize Your Skincare Hub
If your audit points to early-stage surface spots, localized lifestyle friction, or mild pre-period swellings, customized topical chemistry is highly effective. Transitioning to active ingredients that dissolve hardened oil plugs and soothe localized heat will restore clarity while protecting melanin-rich skin from lasting dark marks.
👉 Explore our complete actionable solutions guide for custom routines and native brand formulations.
When to Request Clinical Testing
If your self-audit reveals severe, rock-hard internal swellings that cycle constantly, leave indented marks, or pair with irregular systemic timelines, topical care has reached its functional limit. Consulting a medical professional allows you to investigate root internal causes. When visiting a clinic, consider discussing comprehensive blood panels to test:
- Free and Total Testosterone
- DHEA-S (Dehydroepiandrosterone sulfate)
- Fasting Insulin Levels
- LH/FSH (Luteinizing Hormone to Follicle-Stimulating Hormone) Ratios
Identifying these internal markers ensures you receive the targeted oral or specialist care necessary to calm the oil glands from within.
Q: Can a damaged skin barrier cause my jawline breakouts to look worse?
A: Yes. Overusing harsh, stripping cleansers or applying highly concentrated, raw ingredients to clear a blemish severely depletes your skin's protective moisture mantle. A compromised barrier triggers chronic surface inflammation and leaves the pore openings vulnerable to external bacteria, turning minor blockages into large, angry blemishes.
Q: Why do deep jawline blemishes leave dark patches even if I never pick at them?
A: Melanin-rich skin responds to intense internal inflammation by producing excess pigment to shield and repair the local tissue. Even if you avoid manual squeezing, the sheer depth and pressure of a severe internal blemish stimulate surrounding pigment cells, resulting in Post-Inflammatory Hyperpigmentation (PIH) that requires daily sun protection and gentle, steady renewal to fade smoothly.
Q: Is it possible for heavy hair oils or conditioners to cause breakouts under the chin?
A: Absolutely. Thick, occlusive hair care products and nourishing oils applied to the lengths of the hair easily migrate down the neck and jawline during sleep or while sweating. These formulas can occlude the delicate pores beneath the chin, leading to persistent, smooth surface bumps.